Prostate Cancer
Prostate cancer is an invasive cancer that starts in the prostate, an organ within the typical male reproductive system.1 The prostate surrounds the urethra and produces fluid that, together with testicular sperm cells and other glandular fluids, makes up semen.1 The prostate is approximately the size of a walnut and is located below the bladder and in front of the rectum.1 Prostate cancer is not the same as benign prostatic hyperplasia, which refers to the natural growth of the prostate as someone ages.1
This health awareness social media toolkit can help your cancer control organizations implement evidence-based practices when communicating about prostate cancer.
Data and Statistics
Prostate cancer is the most commonly diagnosed invasive cancer among patients assigned male at birth.2 Approximately 100 per 100,000 patients with male reproductive organs get prostate cancer.2 In addition, prostate cancer is the second-most deadly cancer for patients assigned male at birth across all races and ethnicities.2 Prostate cancer usually occurs in patients aged 65 and older, while cases in those below age 40 are more rare.3 However, survival rates are high for prostate cancer at the localized stage. For all stages of prostate cancer, 96% of patients are still alive five years after diagnosis.1 For men with prostate cancer that has progressed to a distant stage (also known as metastatic prostate cancer), only 34% survive five years after diagnosis.
Treatment options for prostate cancer include surgery, radiation and active surveillance, where the prostate cancer is monitored until there is evidence of cancer progression, at which time treatment may be considered with surgery or radiation.4 About 60% of individuals with low-risk prostate cancer are now managed with active surveillance.5
Best Practices for Communicating About Prostate Cancer
- Address populations that are at higher risk for prostate cancer
-
- Highlight that prostate cancer can be categorized as low-risk, intermediate risk and/or high-risk, based on stage, grading and prostate specific antigen (PSA) levels, a blood test used to screen for prostate cancer.6 These risk groups are important for deciding whether a person can be managed with active surveillance. Furthermore, PSA-based prostate cancer screening is recommended alongside shared decision-making with patients.7
- Encourage providers to recommend screenings for patients with a family history of prostate cancer, since they may be at a greater risk for developing prostate cancer.8
- A family history of prostate cancer includes: (1) people with one brother or father or two or more male relatives with one of the following: (a) diagnosed with prostate cancer at age <60 years; (b) any of whom died of prostate cancer; (c) any of whom had metastatic prostate cancer, (2) Family history of other cancers with two or more cancers in hereditary breast and ovarian cancer syndrome or Lynch syndrome spectrum.9
- Highlight health disparities in cancer incidence and mortality rates among Black and Hispanic people. See “Communicating with Diverse Audiences” below for evidence-based recommendations and sample messages for both Black and Hispanic patients.
- Honor LGBTQI+ patients’ needs while promoting awareness of risks that are specific to transgender individuals. See “Communicating with Diverse Audiences” below for evidence-based recommendations and sample messages for LGBTQI+ patients.
- Acknowledge that risk for prostate cancer increases as a patient ages.8 See “Communicating with Diverse Audiences” below for evidence-based recommendations and sample messages for populations of varying ages.
- Tailor your messages to your intended audience
-
- Share information in an approachable way with simple wording fit for an eighth-grade reading level,10 as older people, those with low income or low education, and immigrant or ethnic/racial minority groups may exhibit lower health literacy, which can contribute to poorer health outcomes.11,12
- Customize your messages and images to your intended audience using tools like Make it Your Own (MIYO). Prostate cancer can potentially be misunderstood and stigmatized among Black and Hispanic patients.13 Address misperceptions via culturally relevant approaches.
- Share risk-reducing options
-
- Emphasize that cancer risk reduction is necessary due to a growing and aging U.S. population. By 2050, the total number of new cancer cases is predicted to increase by almost 50%.14 Prostate cancer is projected to remain one of the top four leading cancers in 2050.14
- Share messaging that recommends tailored dietary practices for prostate cancer survivors. While more research is needed to determine direct links between diet and prostate cancer risk, some studies suggest that diets high in saturated fat, calcium, and dairy intake are associated with increased cancer risk.15
- Remind providers to emphasize the importance of physical activity as part of long-term survivorship care plans. Research shows that physical activity can not only alleviate symptoms like fatigue and depression in cancer survivors, but that at least three hours of exercise per week is also associated with a 61% decrease in prostate cancer mortality.16
- Promote self-advocacy and participation in decision-making
-
- Engage patients in championing their own health. Encourage providers to share toolkits and resources with their patients, especially materials that can be printed and taken to appointments.
- Share information about prostate cancer symptoms to increase patient awareness, self-monitoring and proactive behaviors. Early detection of prostate cancer can allow for timely treatment and reduce risk of death.17
- Share messages that encourage discussion of PSA testing and screening options, particularly with individuals aged 50 years or older. Data from the Health Information National Trends survey found limited communication between patients and providers about prostate-specific antigen (PSA) testing and treatment.18
- Encourage health system improvements to survivorship care and resources
-
- Encourage conversations about fertility and family planning by sharing information and resources providers can share with patients. Cancer treatments such as radiation and chemotherapy can cause short- or long-term impairments in male reproductive organs.19 Surgeries such as prostatectomy often involve the removal of both the prostate gland and seminal vesicles; therefore, patients cannot produce sperm or ejaculate.20
- Make providers aware of resources that can help survivors monitor their health following treatment. Studies indicate that prostate cancer survivors can benefit from personalized health and activity plans provided by digital health technology such as activity trackers.21 Clinical trials can also benefit from the collection of this passive data, which can be difficult to collect from observation alone.21
- Share messages with long- and short-term side effects of prostate cancer treatments and symptom-management resources that patients can consider. Some patients report a lack of information on symptom awareness and management as their survivorship needs evolve.16 Combine these messages with relevant support services wherever possible.
- Provide financial support resources and/or financial navigation as several cancer treatment medications used to treat late-stage prostate cancer can be relatively expensive.22
- Refer prostate cancer patients to clinical trials
-
- Although prostate cancer survivors account for 20% of the survivorship population, prostate cancer and prostate cancer survivors are the subjects of only 5% of research.23 Messages that remind providers to engage survivors in clinical research can help to address this gap.
Communicating with Diverse Audiences
Communication-related issues may also play a role in cancer disparities.24 Consider the information most useful to each diverse group (see below for specific messaging and read more on health disparities here). Tailor communication to these populations of focus with messages that also address conditions where these communities live, learn, work and play, as these social determinants of health can impact a wide range of health risks and outcomes. To ensure messages resonate with the coalition’s intended audience, we also recommend referring to the National Networks’ existing resources and adapting messages to reflect individuals with lived experiences.
- Black/African American
-
- Compared to other racial/ethnic groups, Black persons are the most likely to be diagnosed with prostate cancer. Age-adjusted data up to 2020 showed 155 new prostate cancer cases among Black patients versus 95 new cases among White patients per 100,000. Moreover, Black patients are more likely to die from prostate cancer than non-Hispanic White patients.2 Draw attention to these health disparities in messages and promote tailored efforts to increase screenings and symptom awareness for Black persons.
- Black persons are diagnosed with prostate cancer at younger ages and experience higher rates of advanced prostate cancer.8 Share messages that encourage providers to assess risk of prostate cancer for Black persons, particularly those with a family history of prostate cancer, to better inform screening timelines.
- LGBTQI+
-
- LGBTQI+ patients and survivors report fears of social stigma as well as experiencing stigma within health care settings.25 Create messages that help health providers recognize and overcome implicit bias when communicating with patients with prostate cancer. This may help to reduce stigma and to foster trust and honesty.
- Transgender people with male reproductive organs have varying risk levels based on their history with gender-affirming surgery (GAS) and gender-affirming hormone therapy (GAHT).26 Patients who have not undergone GAS or begun GAHT have the same risk levels as cisgender patients with male reproductive organs.26 However, patients with a history of GAS or GAHT are less likely to get prostate cancer than their age-matched cis-male counterparts.26 Share these trends in your messaging to providers.
- Research shows no correlation between anal sex and increased risk of prostate cancer.27 However, removal or damage of the prostate due to cancer treatment may affect a patient’s sexual function and/or desire. If appropriate, connect LGBTQI+ patients with sex therapists or support groups to discuss these potential changes. The GW Cancer Center’s Living with Prostate Cancer guide contains more information on adapting one’s sex life and other changes after treatment.
- Hispanic/Latinx/o/a
-
- Children of Hispanic parents who identify as a prostate cancer survivor are more likely to understand their own increased risk for prostate cancer and desire information and support from their parents.28 However, cultural taboos surrounding discussions of sex and intimacy between parents and children often discourage conversations on prostate cancer screening and risk.28 Share messages that encourage healthcare professionals to encourage Hispanic parents who are prostate cancer survivors to serve as mentors for their own families. Messages can also empower providers to share cancer screening and risk information to Hispanic children.28
- AANHPI (Asian American, Native Hawaiian/Pacific Islander)
-
- Prostate cancer is the leading cancer diagnosis among AANHPI men (50 cases per 100,000).2
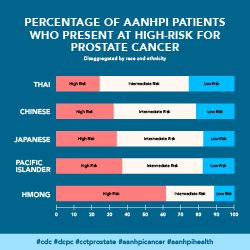
- Although some studies indicate lower incidence of prostate cancer among AANHPI persons compared to other racial/ethnic groups,29 there is limited research available that disaggregates AANHPI into further subgroups, which demonstrate varying levels of risk when studied independently.30 For example, Hmong patients have a higher risk of disease when compared to Chinese patients.30
- AANHPI subgroups also vary in their rates of receiving treatment and having their health actively surveilled.30 For example, Kampuchean patients are less likely to receive treatment than Hmong or Hawaiian patients.30 Avoid messaging that aggregates these demographics. Instead, share data and recommendations tailored to a clearly stated subgroup. Providers can also engage AANHPI patients in future research that assesses prostate cancer risks among the many different subgroups.
- AI/AN (American Indian/Alaska Native)
-
- Compared to Black persons, White persons, and Asian Americans, AI/AN individuals experience the highest rates of late-stage prostate cancer and cancer mortality. However, they are less likely to receive optimal treatment, which may be due to reduced access to specialty care in certain areas.31 Use this data in messages to promote screenings within this community. Providers can also share virtual health options for AI/AN persons residing in rural areas.
- Age-based messaging
-
- Share age-appropriate screening information, as age is the most common risk factor in getting prostate cancer.8 Patients between 55-69 should talk with their provider to determine if screening is right for them. Screening for patients older than 70 is not recommended by the U.S. Preventive Services Task Force.32
Prostate Cancer Messages and Graphics
Download All Messages and Graphics How to Post on Social Media
|
Topics |
Suggested Images |
|---|---|
|
Topic: Resources for newly diagnosed patients #cdc #dcpc #cctprostate |

|
|
Topic: Share information about prostate cancer symptoms #cdc #dcpc #cctprostate |

|
|
Topic: Engage patients in creating a survivorship care plan #cdc #dcpc #cctprostate #cancersurvivor |

|
|
Topic: Share prostate cancer resources that patients can use to guide conversations with their providers #cdc #dcpc #cctprostate #prostatecancer |

|
|
Topic: Share information about prostate cancer health disparities for Black patients #cdc #dcpc #cctprostate #blackhealth |

|
|
Topic: Share information on family history #cdc #dcpc #cctprostate |

|
|
Topic: Provide education on long-term side effects of treatments #cdc #dcpc #cctprostate |

|
|
Topic: Empowering Hispanic parents who are prostate cancer survivors to share information with their children #cdc #dcpc #cctprostate #hispaniccancer #hispanichealth |

|
|
Topic: Address fertility risks caused by prostate cancer treatment and provide resources for fertility preservation #cdc #dcpc #cctprostate #cancerfertility |

|
|
Topic: Promote risk-reducing behaviors and practices #cdc #dcpc #cctprostate |

|
|
Topic: Tips for caring for LGBTQI+ patients #cdc #dcpc #cctprostate #lgbtcancer |

|
|
Topic: Tips for caring for transgender patients #cdc #dcpc #cctprostate #lgbtcancer #transhealth |

|
|
Topic: Prostate cancer risks for transgender patients #cdc #dcpc #cctprostate #lgbtcancer #transhealth |

|
|
Topic: Support groups for prostate cancer patient and survivors #cdc #dcpc #cctprostate |

|
|
Topic: Referring patients to clinical trials #cdc #dcpc #cctprostate #cancertrials |

|
|
Topic: Make providers aware of disparities in risk and treatment for Asian American Native Hawaiian Pacific Island (AANHPI) patients #cdc #dcpc #cctprostate #aanhpicancer #aanhpihealth |
|
|
Topic: Policy Systems Environment (PSE) change #cctprostate #cdc #dcpc #healthyeating #PSEchange |

|
|
Topic: Different risk groups for prostate cancer #cdc #dcpc #cctprostate |

|
Download All Messages and Graphics How to Post on Social Media
How to Post to Social Media
Start by downloading the ZIP file above. Then double click the downloaded file to unzip and open the folder. Inside, you’ll find four CSV files.
- Messaging.csv contains captions for all messages in the toolkit, organized by topic.
- Bulk - Instagram.csv contains captions for all Instagram messages, along with graphics URLs that can be used to bulk schedule both text and images.
- Bulk - LinkedIn-Facebook-Twitter.csv contains captions for all LinkedIn, Facebook, and Twitter messages, along with graphics URLs that can be used to bulk schedule both text and images.
- Bulk - Twitter.csv contains captions for all Twitter messages, along with graphics URLs that can be used to bulk schedule both text and images.
Inside the main folder, you’ll also see two sub-folders containing the messaging graphics for all major platforms. The first folder contains rectangular images suited for use on Facebook, Twitter, and LinkedIn. The second folder contains square images suited for Instagram.
Select your platform below for additional instructions.
-
- Download the suggested graphic.
- Highlight the corresponding message with your cursor. Right click and select “Copy.”
- Open Facebook. If you aren’t already logged in, enter your email address (or phone number) and password, then tap “Log in.”
- Tap the post box. This box is at the top of the News Feed. If you're posting to a group, you’ll find the box just below the cover photo. There will generally be a phrase like “Write something”or “What’s on your mind?” in the box.
- Tap “Photo/Video” near the middle of the post screen, then select the downloaded graphic to upload and tap “Done.” Doing so adds the photo to your post.
- Tap “Post.” It’s in the top-right corner of the screen from the app, or the bottom-right from your computer. Doing so will create your post and add it to the page you’re on.
-
- Download the suggested graphic.
- Highlight the corresponding message with your cursor. Right click and select “Copy.”
- Open Twitter. If you aren’t already logged in, enter your email address and password, then tap “Log in.”
- Tap the post button. This button is at the bottom right of the News Feed. There will generally be a phrase like “What’s happening?” in the box.
- Tap the camera icon near the middle of the post screen, or the picture icon in the bottom left of the post screen then select the downloaded graphic to upload, and add the post caption.
- Tap “Tweet.” It’s in the top-right corner of the screen from the app, or the bottom-right from your computer. Doing so will create your post and add it to the page you’re on.
-
- Download the suggested graphic.
- Highlight the corresponding message with your cursor. Right click and select “Copy.”
- Open Instagram. If you aren’t already logged in, enter your username (or phone number) and password, then tap “Log in.”
- Tap the plus sign box. This box is at the top right. Select the downloaded graphic or drag it into the box to upload it.
- Select “Square (1:1)” for the aspect ratio, then click “Next.”
- Ignore the filters screen, then click “Next” again.
- Paste the caption where it says, “Write a caption…” at the top.
- Under “Accessibility,” consider adding alt text to describe the photo for people with visual impairments.
- Tap “Share.” It's in the bottom-right corner of the screen.
-
- Download the suggested graphic.
- Highlight the corresponding message with your cursor. Right click and select “Copy.”
- Open LinkedIn. If you aren’t already logged in, enter your email address and password, then tap “Log in.”
- Tap “Start a post” from the main share box. This box is at the top of your profile.
- Tap “Photo” from the top of the post screen, then select the downloaded graphic to upload and tap “Done.” Doing so adds the photo to your post.
- Tap “Post.” It's in the the bottom-right. Doing so will create your post and add it to the page you’re on.
- Bulk Scheduling
-
Social media management tools like Hootsuite and Sprout Social offer bulk scheduling options for uploading multiple messages at once. The spreadsheets included in the download can be adapted to fit multiple scheduling platforms or services. They are currently formatted to work with Sprout Social’s bulk scheduling option. Please review the bulk scheduling format requirements for your specific platform before posting. Messages are sorted by network.
Prostate Cancer Resources
|
Resource |
Description |
|---|---|
| ZERO Prostate Cancer | Advancing prostate cancer awareness and working to end health disparities affecting Black patients. ZERO also connects patients and mentors to financial resources, support groups, and educational resources, with some specific to Black patients and LGBTQ+ patients. |
| CancerCare Gynecological Cancers Patient Support Group | A free, 15-week support group for patients living with gynecological cancer who are currently in treatment. |
| Prostate Cancer Research Institute | Providing science-based data and research to help prostate cancer patients and caregivers gain insight and understanding. |
| CancerCare Prostate Cancer Patient Support Group | Offering a free, 15-week virtual support group led by an oncology social worker to help patients connect and cope. |
| Urology Care Foundation | Providing information about symptoms, diagnosis, treatment, and more, in addition to a podcast series for caregivers of people with prostate cancer. |
| Prostate Cancer Foundation | Funding research that advances the prevention, detection, and treatment of prostate cancer, as well as providing materials such as patient guides and financial resources. |
| Prostate Health Education Network | An organization working to eliminate the disparities African Americans experience in prostate cancer through policy, outreach, and community building. |
| Make it Your Own | A tool for helping medical professionals to create tailored health communications with evidence-based messaging and customized images. |
| National Cancer Institute | Providing resources for both patients and providers to help them understand prostate cancer, treatments, screenings, and statistics. |
| Prostate Cancer Clinical Trials Consortium | An organization dedicated to improving standards of prostate cancer care through process-driven clinical trials. |
| National LGBT Cancer Network | Improving the lives of LGBTQ+ cancer survivors through advocacy, education, and training. |
| Gay and Lesbian Medical Association | A group dedicated to ensuring health equity for LGBTQ+ people through research, advocacy, and education. GLMA also shares resources for both patients and providers caring for LGBTQ+ people. |
| Talk to Nathan | A CDC resource that provides interactive conversations for both patients and providers to help make decisions about prostate cancer screening and/or treatment. |
| Florida Prostate Cancer Advisory Council | Reliable source of prostate cancer information that is accessible to patients, advocates, physicians, care providers, researchers and Florida’s governing officials. |
| American Urological Association | New guidelines released as of 2023 on Early Detection of Prostate Cancer |
| American Urological Association | New guidelines released as of 2023 on Early Detection of Prostate Cancer |
| National Comprehensive Cancer Network | New guidelines for clinical management of prostate cancer |
References
